Pregnancy is a remarkable journey, filled with excitement, happiness, and physical changes. While the joy of expecting a child is immense, the physical discomforts that accompany pregnancy can sometimes overshadow this happiness. Among these discomforts, neck pain is a common issue that many pregnant women experience. Understanding the causes of neck pain during pregnancy and learning how to alleviate it can significantly improve your comfort and overall well-being during this special time. To know more about this information read the whole blog which is going to explain those in detail in an understandable manner.
Causes of Neck Pain during Pregnancy:
Hormonal Changes:
During Pregnancy, Your body undergoes major hormonal changes particularly hormonal release called progesterone and relaxing. These hormones help to loosen the ligaments and joints in the pelvis regions to prepare your body for childbirth. However, it also affects other joints including the neck. This increased flexibility can lead to discomfort and neck pain during pregnancy.
Postural Changes:
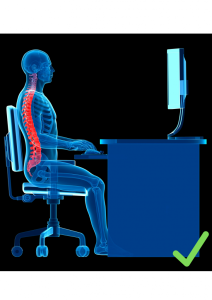
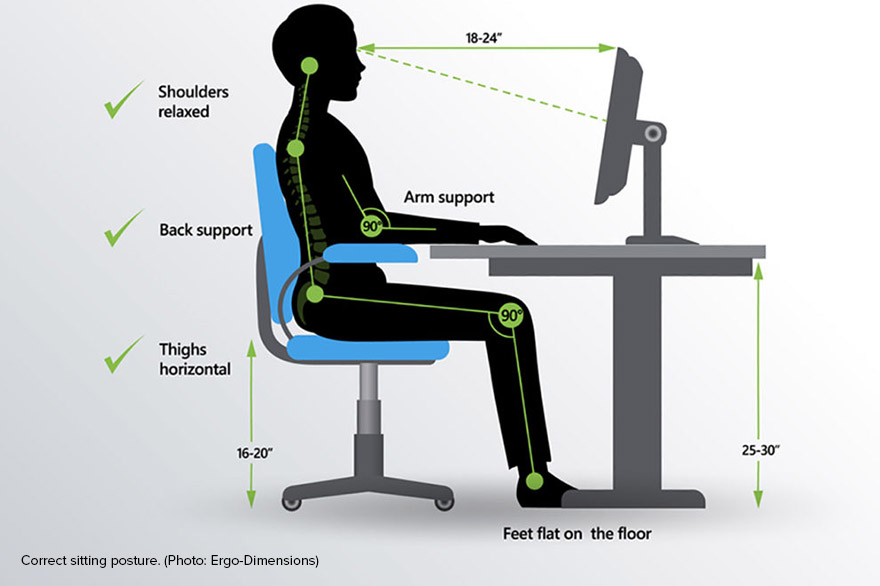
As the belly grows, pregnant women often experience back and neck pain. A major contributing factor to this discomfort is poor posture, such as hunching over a phone or while working at a desk.
Weight Gain:
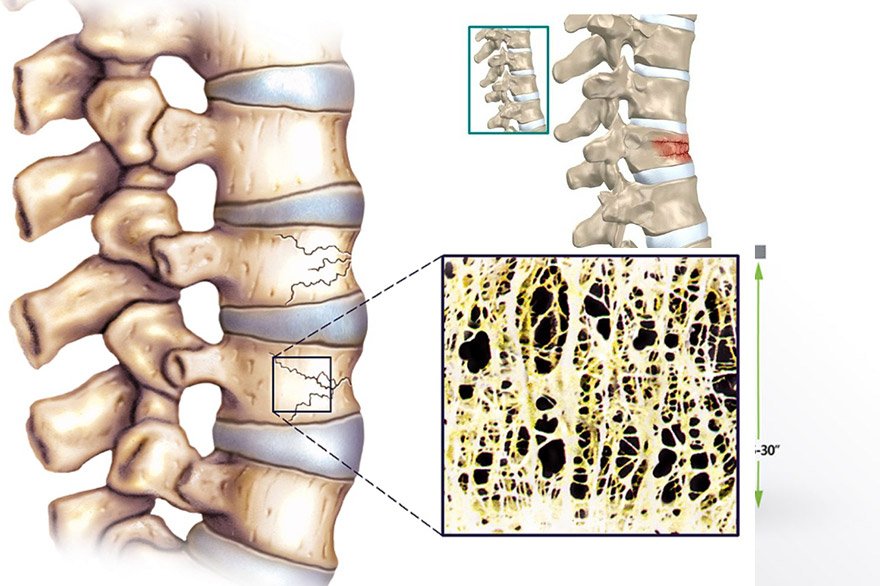
The natural weight gain during pregnancy, while essential for the baby’s development, also puts additional pressure on the spine. The increased weight can cause muscles, especially in the neck and back, to work harder to support the body, leading to fatigue and pain.
Sleep Discomfort:
As pregnancy progresses, finding a comfortable sleeping position becomes more challenging. Many pregnant women find themselves sleeping in positions that strain the neck, such as lying on the back with inadequate support. Poor sleep posture can contribute to morning neck stiffness and pain.
Effective Ways to Alleviate Neck Pain:
Prenatal Exercises and stretches:
Engaging in regular gentle exercise can strengthen your neck muscles and reduce pain. some effective exercises include:
- Slowly tilt your head towards your shoulders, holding for a few seconds on each side.
- Gently pull your chin towards your chest, holding for a few seconds before releasing.
- Roll your shoulders backward and forward to relieve tension.
Techniques for Stress Management:
Effective stress management throughout pregnancy can ease neck pain and ease tense muscles. Think about implementing relaxing methods like:
- Prenatal yoga: Encourages relaxation while strengthening and extending the body.
- Stress reduction and mental calmness are the main goals of meditation.
- Practices including deep breathing can help release tension in the shoulders and neck.
- It’s important to prioritize your mental health and take some time to relax during pregnancy.
Therapy with Heat and Cold:
Neck discomfort can be effectively relieved with hot and cold therapy. This is how to apply them:
- Cold Compress: To ease discomfort and reduce inflammation, place a cold compress on the neck for 10 to 15 minutes.
- Hot Compress: To relieve tight muscles after the acute inflammation goes down, use a warm compress or take a warm shower.
To prevent burns or frostbite, always place a towel between the compress and your skin.
Final thought:
Although many women suffer neck pain during pregnancy, it doesn’t have to be an essential part of the experience. Pregnancy can be more comfortable and healthful if you are aware of the reasons for neck pain and take steps to reduce it. Never forget how crucial it is to put self-care first and ask for help when you need it.
Do not be afraid to seek advice and direction from your healthcare provider in neck pain treatment in Bangalore if you are experiencing neck pain during pregnancy. Being proactive in managing and preventing pain can have a big impact on how your pregnancy goes. Neck pain treatment at Bangalore hospitals, such as Neurowellness, can help alleviate your pain.
If you’re seeking the best neck pain treatment in Bangalore, contact Neurowellness for personalized care and attention.