By Dr. Ganesh Veerabhadraiah — Neurosurgeon & Interventional Neuroradiologist, Kauvery Hospital, Electronic City, Bengaluru
Most Text neck pain in Bengaluru today is not a disc problem — it is muscle spasm caused by poor posture from mobile phones, laptops, bean bags and work-from-home setups. The condition is widely known as text neck. In the majority of cases, it is reversible without surgery through posture correction, ergonomic changes and short-term medical management.
If you are an IT professional, student, or remote worker in Bangalore experiencing persistent neck pain, this guide explains the real causes, warning signs, and what actually works — based on patients I treat every week at my Electronic City clinic.
Worried your neck pain isn’t going away?
Get a proper evaluation before it becomes chronic.
What Is Text Neck?
Text neck is a repetitive strain injury of the cervical spine caused by long hours of looking down at smartphones, laptops, tablets, and microscopes.
When your head sits upright over your shoulders, your neck muscles handle its weight (about 5 kg) easily. But when you tilt your head forward by just 45 degrees to read a phone, the effective load on your cervical spine jumps to nearly 22 kg. Sustained over hours every day, this triggers:
• Muscle fatigue and spasm
• Ligament strain
• Loss of the neck’s natural curve (cervical lordosis)
• Chronic pain, stiffness and headaches
The important clinical point most text neck cases are muscular, not structural. That changes everything about how it should be treated.
Why Neck Pain in Bangalore Is Now a Daily Complaint
Bengaluru’s lifestyle is a near-perfect recipe for cervical strain. In my own practice across Electronic City, Whitefield, Koramangala and HSR Layout, the common patient profiles include:
• IT and software professionalsspending 9–12 hours on dual monitors
• Startup founders and remote workersusing laptops on beds, sofas and bean bags
• Students and exam-prep candidatesglued to mobile screens
• Mobile and electronics techniciansworking under microscopes
• Gig workers and content creators scrolling for hours
This is why cervical pain in IT professionals in Bangalore has become one of the most frequent reasons for neurosurgery consultations in the city and why awareness of text neck matters more than ever.
A worrying trend I see: most professionals delay treatment for months, hoping the pain will “go away on its own”. I’ve explained the consequences of this in detail in my earlier post on why Bengaluru professionals delay back pain treatment and why it’s risky the same pattern applies to neck pain.
What Causes Neck Muscle Spasm? The Real Story
Most patients walk in worried about disc prolapse, pinched nerves, or surgery. But when I examine them, the actual neck muscle spasm causes turn out to be everyday lifestyle habits:
Habit | Why It Damages Your Neck |
Working on a laptop in bed | Neck bent forward, no spine support |
Sitting on bean bags for hours | Pelvis sinks, neck juts forward to see screen |
Sleeping on a sofa | Awkward angles for prolonged hours |
Looking down at the phone | 45° flexion = ~22 kg load on cervical spine |
Improper weight lifting at the gym | Sudden force on already fatigued muscles |
Microscope or precision work | Continuous static forward bend |
Individually these feel harmless. Stacked across months and years, they produce the exact pattern I see on most cervical X-rays straightening of the spine and sustained muscle spasm.
What Is "Straightening of the Cervical Spine"?
A healthy neck has a gentle inward curve called cervical lordosis. When neck muscles stay tight for long periods, they pull this curve flat. Radiologists report this as “straightening of the cervical spine” on your X-ray or MRI.
Is straightening of the cervical spine serious?
In most cases no. It is a sign that your muscles are spasming and your posture has been poor, not that your spine is structurally damaged. The good news:
• It is reversiblein early and moderate stages
• Straightening of the cervical spine treatmentis mostly non-surgical
• Posture correction + targeted exercises + short-term medication restore the curve in most patients
Surgery is reserved for the rare cases where there is genuine nerve compression, weakness, or progressive neurological symptoms not for muscle spasm. If you are confused by your scan report, my guide on understanding your MRI scan results walks through what each finding really means.
Real Patient Cases From My Bengaluru Practice
The clearest way to explain text neck is to share two recent cases from my own clinic.
Case 1 – The IT Professional and the Bean Bag
A 32-year-old software engineer came to me about two weeks ago with months of severe neck pain and stiffness. He had already tried painkillers, traction, and chiropractic adjustments. Nothing worked.
On evaluation:
• X-ray showed straightening of the cervical spine
• No significant disc problem
• No nerve compression
The hidden cause: He had been working from home on a bean bag for 8–10 hours every day, often slipping into a half-lying position with his laptop on his chest. His neck was constantly bent in unnatural angles.
What actually worked:
• Strict posture correction (proper desk, chair, screen height)
• Stopping bean bag use for work
• A short course of muscle relaxants and anti-inflammatories
• Daily neck mobility exercises
He is now significantly improved, working pain-free, and back to normal life without any procedure.
Case 2 – The Mobile Repair Technician
A mobile repair technician came in with long-standing severe neck pain. His work involves bending forward under a microscope to work on tiny circuit boards for hours every day.
He had already done MRI, X-ray and CT all clear of any major structural issue, except again, straightening of the cervical spine.
What helped him recover:
• Ergonomic adjustments at his workbench (raised microscope, supported chair)
• Scheduled micro-breaks every 30 minutes
• Targeted physiotherapy Short-term medical management
He is steadily recovering without surgery, without injections.
The lesson from both cases: the posture decides spine health, not the technology.
Recognise yourself in either of these stories?
You don’t need to live with daily neck pain. A 30-minute consultation can identify exactly what’s wrong and put a non-surgical recovery plan in place.
Symptoms of Text Neck - When to Take It Seriously
Early symptoms (lifestyle-stage)
• Neck stiffness on waking
• Dull ache at the base of the neck
• Tightness in the shoulders and upper back
Progressive symptoms
• Frequent tension headaches
• Pain radiating to the upper back
• Reduced ability to turn the head fully
Red-flag symptoms — see a neurosurgeon
• Pain shooting down the arm
• Numbness or tingling in the fingers
• Weakness in grip or hand muscles
• Loss of fine hand control (dropping objects, fumbling buttons)
If you have any red-flag symptoms, do not self-treat. These suggest possible nerve involvement and need clinical evaluation.
Have any red-flag symptoms?
Don’t wait. Early evaluation prevents permanent nerve damage.
Mobile Neck Pain Prevention - A Practical India Guide
These are the same instructions I give my patients every week. They are simple, free, and effective.
1. The Eye-Level Rule
Bring your phone up to eye level instead of bending your head down. Even 30° less flexion dramatically reduces cervical load.
2. Fix Your Workstation
• Top of the monitor should sit at or slightly below eye level
• Feet flat, hips and knees at 90°
• Forearms parallel to the floor
• Use an external keyboard and mouse if you work on a laptop
3. Stop Using the Laptop in Bed
This is the single most common cause of work from home neck pain I see in Bengaluru. The neck has no way to stay neutral in a bed setup.
4. Avoid Bean Bags and Sofas for Work
Comfort is not the same as posture. Anything that lets your pelvis sink will force your neck forward.
5. Follow the 20-20-20 Rule
Every 20 minutes, look at something 20 feet away for 20 seconds. Stand up and roll your shoulders every hour.
6. Daily Neck Exercises (5 minutes is enough)
• Chin tucks— 10 reps, 3 sets
• Gentle neck extensions— 10 reps
• Side bends— 10 each side
• Shoulder rolls— 10 forward, 10 backward
7. Lift Weights Carefully
Avoid jerky movements. Keep the neck neutral, never crane forward to check form in the mirror.
8. Sleep Right
Use a single, medium-firm pillow that keeps the neck aligned with the spine. Side sleepers may need slightly thicker support, back sleepers thinner.
Text Neck Treatment in Bengaluru — What Actually Works
Most patients improve completely with a non-surgical approach. The standard text neck treatment plan in Bengaluru clinics, including mine, looks like this:
Phase 1 – Pain control (1–2 weeks):
• Short course of muscle relaxants and anti-inflammatories
• Hot fomentation
• Activity modification
Phase 2 – Recovery (2–6 weeks):
• Posture correction
• Physiotherapy and structured neck exercises
• Ergonomic redesign of workstation
Phase 3 – Long-term protection:
• Daily exercise routine
• Lifestyle changes around screen time
• Follow-up review if symptoms return
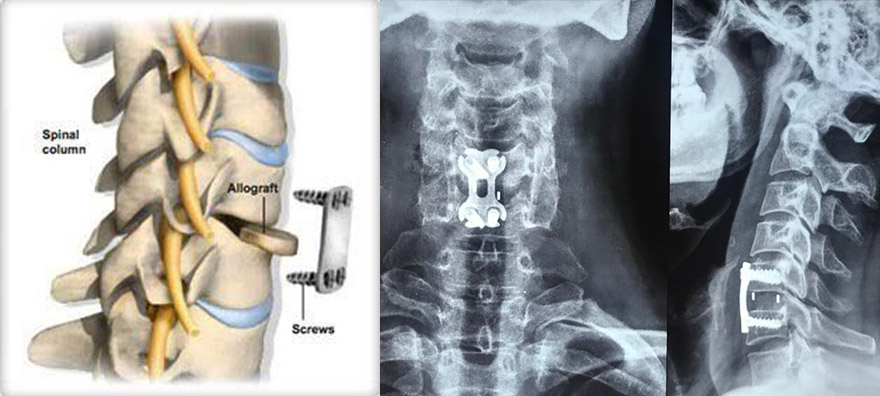
When Is Surgery Needed?
Surgery for neck pain is rare and only considered when:
• An MRI confirms significant disc prolapse with nerve compression
• The patient has progressive arm weakness or numbness
• Conservative treatment for several weeks has failed
• There are signs of cord compression (myelopathy)
For pure text neck and muscle spasm cases, surgery is not the answer. I’ve written a detailed honest guide on whether you really need spine surgery please read it before agreeing to any procedure. When surgery is genuinely required, modern techniques like minimally invasive spine surgery make recovery much faster than older approaches.
Daily Spine Care Checklist
☐ Sit upright with both feet flat on the floor
☐ Top of screen at eye level
☐ No laptop work on the bed
☐ No bean bag for working hours
☐ Phone at eye level, not on the lap
☐ Break and stretch every 60 minutes
☐ 5 minutes of neck exercises daily
☐ Sleep on a supportive pillow
Frequently Asked Questions
1. Is text neck a serious medical condition?
Text neck is mostly a muscular and postural condition. It is not dangerous in early stages, but if ignored for years it can accelerate cervical disc wear and contribute to chronic pain. Early correction prevents long-term damage.
2. Can text neck be cured permanently?
Yes — in most cases. When the underlying postural habits are corrected and muscle spasm is treated, the cervical curve and pain resolve. Recurrence happens only if old habits return.
3. How long does it take to recover from text neck?
Mild cases improve in 2–4 weeks with posture correction and exercises. Moderate cases may take 6–12 weeks. Cases with long-standing spasm and straightening of the cervical spine can take a few months but still recover without surgery.
4. Do I need an MRI for neck pain?
Not always. For routine neck pain without red-flag symptoms, a clinical examination and X-ray are usually enough. MRI is reserved for cases with arm pain, numbness, weakness, or failure of conservative treatment. For a clearer understanding of what scan reports mean, see MRI scan results explained by a neurosurgeon.
5. Is text neck reversible?
Yes. Loss of the cervical curve and muscle spasm are reversible in most patients through posture correction, physiotherapy, ergonomic changes and short-term medication. Surgery is rarely needed.
6. Which doctor should I see for neck pain in Bangalore?
For simple posture-related pain, a physiotherapist or general physician is a reasonable first step. If you have severe pain, radiating arm pain, numbness, weakness, or pain that has not improved in 2–3 weeks, consult a neurosurgeon or spine specialist for a proper evaluation. You can book directly with Dr. Ganesh Veerabhadraiah at our Electronic City or Jayanagar clinics.
7. Is work from home causing more neck pain in India?
Yes — significantly. Improper home setups, laptops on beds, sofas and bean bags, and longer screen hours have produced a sharp rise in cervical strain, particularly among IT professionals in Bengaluru, Hyderabad, Pune and Gurugram.
8. Can neck pain cause headaches?
Yes. Tight muscles at the base of the skull (suboccipital muscles) commonly refer pain to the back of the head, temples and behind the eyes. Many “chronic headaches” are actually cervicogenic.
Take Control of Your Spine Health
Text neck is real, but it is also one of the most preventable spine problems of our time. The encouraging clinical truth is this:
• Most cases do not need surgery
• Most cases improve with posture and lifestyle correction
• Early intervention almost always works
If you have been struggling with persistent neck pain, do not panic but do not ignore it either. A proper evaluation will tell you exactly what is happening and what to do next.
Consult Dr. Ganesh Veerabhadraiah — Neurosurgeon, Bengaluru
Neurosurgeon & Interventional Neuroradiologist
Kauvery Hospital, Electronic City, Bengaluru
📞 +91 7259669911 (Jayanagar) | +91 7411571002 (Electronic City)
Book your consultation today
✅ Spine specialist in Electronic City
✅ Spine specialist in Jayanagar
✅ Get a second opinion on existing scans
Early evaluation prevents long-term damage. Don’t let “manageable” neck pain become a chronic spine problem.