Lower back pain may be caused by spondylolisthesis, a spinal disorder. It happens when one of your vertebrae or spine bones slips out of place and lands on the vertebra below it. Nonsurgical treatment can usually alleviate your problems. In most cases, surgery for severe grade spondylolisthesis is effective.
What is spondylolisthesis?
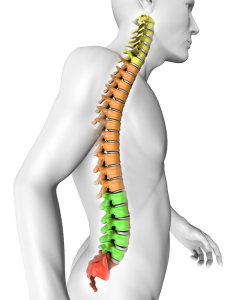
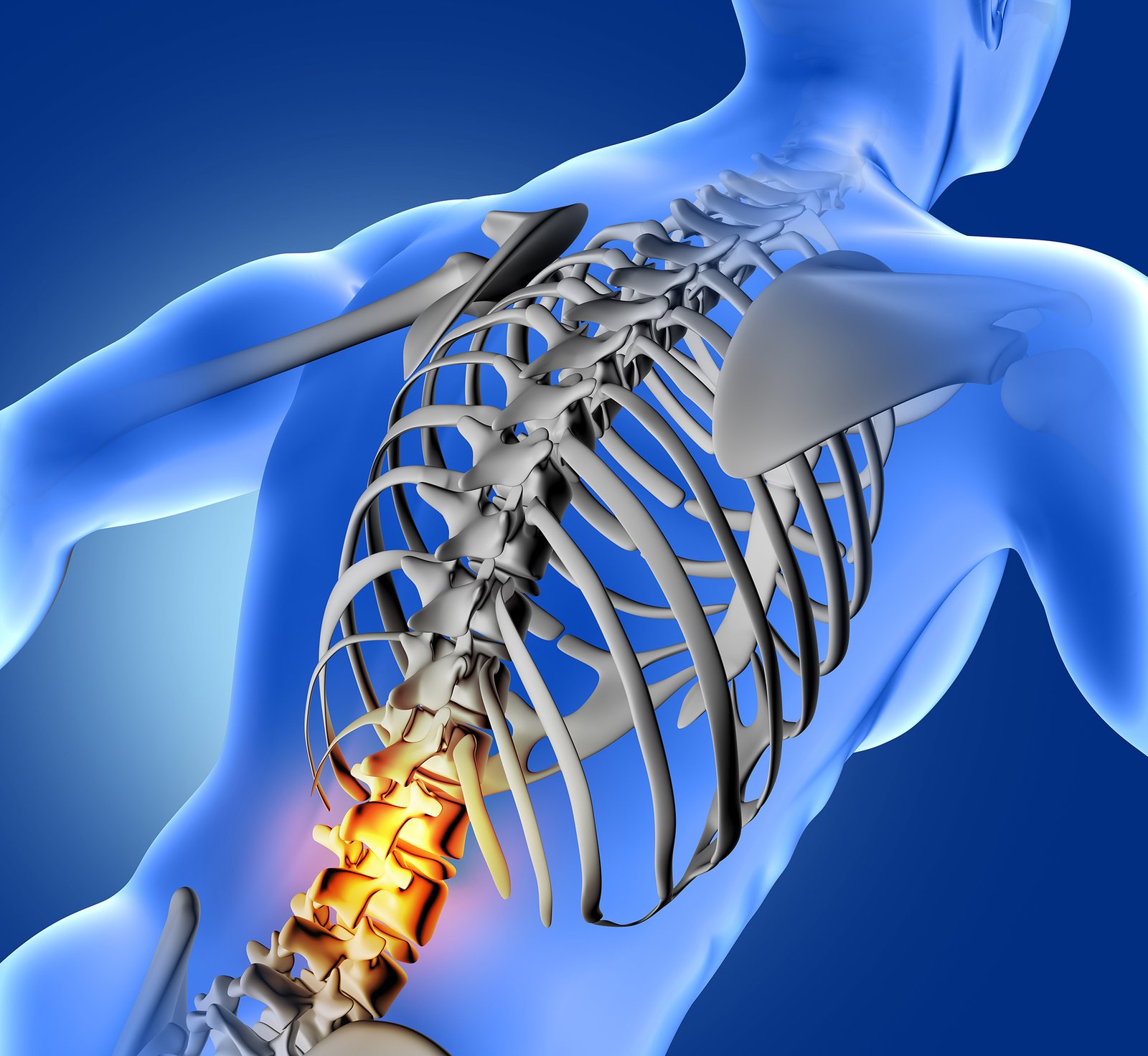
Spondylolsthesis is a condition in which the vertebrae move more than they should, resulting in spine instability. A vertebra slips out of place and lands on the one below it. There will be pars interarticularis defect a bone connecting upper and lower facet. It could exert pressure on a nerve, resulting in lower back or leg pain.
The Greek words spondylos, which means “spine” or “vertebra” and listhesis, which means “slipping, sliding or moving” are combined to form spondylolisthesis (pronounced sphon-di-low-less-THEE-sis).
Types of spondylolisthesis:
- Degenerative spondylolisthesis: the most prevalent kind is degenerative spondylolisthesis, which occurs as a result of ageing.
- Isthmic spondylolisthesis: as a result of spondylolisthesis, isthmic spondylolistheis develops. The bone is weakened by the crack or fracture.
- Congenital spondylolisthesis: when a baby’s spine does not form properly before birth, this is known as congenital spondylolisthesis. The person’s vertebrae are misaligned, putting them at risk for slippage later in life.
- Less common types of spondylolisthesis are:
- Traumatic spondylolisthesis: it occurs when the vertebrae slip as a result of an injury.
- Pathological spondylolisthesis: when a disease, such as osteoporosis, or a tumour, develops pathological spondylolisthesis.
- Post surgical spondylolisthesis: slippage as a result of spinal surgery is known as post-surgical spondylolisthesis.
How common is spondylolisthesis?
Spondylolisthesis and spondylolysis affect approximately 4% to 6% of the adult population. It is easy to go years without realising you have spondylolisthesis because you do not have any symptoms.
Degenerative spondylolisthesis (which happens as a result of ageing and wear and tear of the spine) is more common in women than in men after the age of 50.
Isthmic spondylolisthesis (typically induced by spondylolysis) is one of the most common reasons for back pain in teenagers.
Causes of spondylolisthesis:
One of the most common causes of spondylolisthesis in young athletes is overextending the spine. Genetics could also have a role. Some people are born with spinal bones that are thinner than others. Wear and tear on the spine and discs (the cushions between the vertebrae) can develop this problem in older persons.
What are the symptoms of spondylolisthesis?
You might not notice any signs or symptoms of spondylolisthesis. Some people are unaware that they have the disease. If you do experience symptoms, the most common one is lower back ache. The discomfort may spread to the buttocks and thighs. You may also experience:
- Back pain/leg pain aggravated by activity- working at home or bending and picking up object.
- Stiffness in the back
- Spasms in the hamstring muscle (muscles in the back of the thighs)
- Walking or standing for long periods of time is difficult
- When leaning over, there is pain
- Numbness, tingling or weakness in the foot.
How is spondylolisthesis diagnosed?
Your doctor will conduct a physical examination and inquire about your symptoms. An imaging/scan will very certainly be required to confirm the diagnosis.
What imaging tests will be needed?
- A spinal X ray allows doctors to see if a vertebrae is misaligned.
- To see the spine in greater detail or to see soft tissue like discs and nerves, a CT scan or an MRI scan may be required.
How to reduce the risk of spondylolisthesis?
You can lower your chance of spondylolisthesis by doing the following:
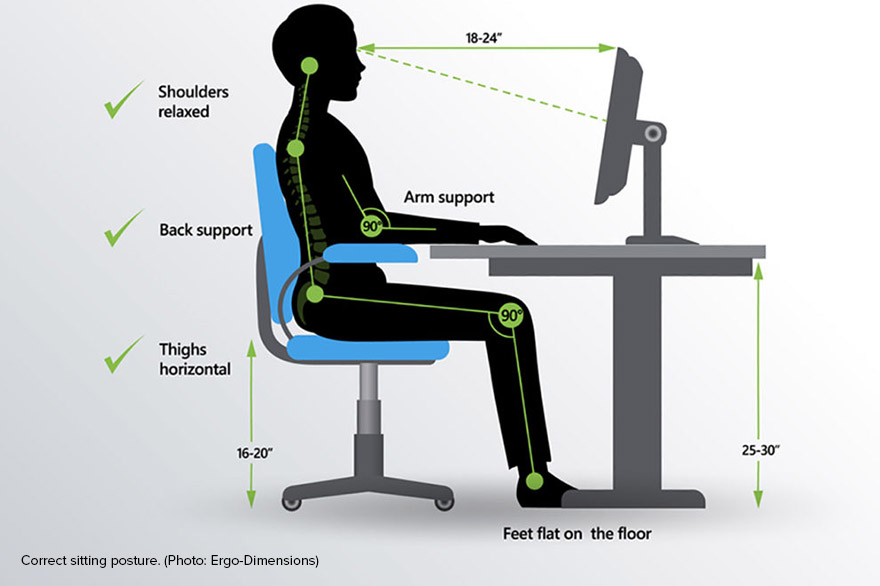
- Regularly exercise your back and abdominal muscles to keep them strong
- Maintain a healthy body mass index (BMI). Weight gain puts additional strain on your lower back
- To keep your bones well nourished and robust, eat a well balanced diet.
What is the outlook for people with spondylolisthesis?
The success rate of surgery is very high. Spondylolisthesis surgery patients typically return to an active lifestyle after a few months following surgery. Following surgery, you will almost certainly require therapy to help you regain full function.
Summary:
Spondylolisthesis is one of the common cause of back pain /discomfort, however it is not life threatening. There are a variety of therapists available, ranging from medicine to physical therapy to spinal surgery. If you are experiencing low back discomfort or finding it difficult to walk, stand, or bend over, consult the Neuro Wellness Care Center, they will provide the best and cost friendly Back Pain Treatment in Bangalore.