Spinal tuberculosis treatment in Bengaluru becomes critical when delayed diagnosis leads to spinal cord compression and paralysis. This case of a 65-year-old patient demonstrates how advanced Pott’s spine surgery in India, including thoracic spinal cord compression treatment and lumbar canal stenosis L4-L5 surgery, restored neurological function after emergency spine surgery in Bengaluru.
Spinal tuberculosis, also called Pott’s spine, can silently destroy vertebral bones, compress the spinal cord, and cause irreversible disability if not treated early by a spine infection specialist in Bengaluru.
Spinal tuberculosis (Pott’s spine) remains a significant health concern in India. While many patients initially present with back pain alone, delayed diagnosis and treatment can lead to devastating neurological complications, including paralysis.
This case highlights the importance of early recognition and timely surgical intervention in spine infections.
What Was the Initial Presentation?
Severe Upper Back Pain
The patient reported:
• Severe upper back pain for 3–4 months
• Band-like pain radiating around the chest
• Pain worsening on coughing and sneezing
• No weakness initially
• No numbness
• No bladder or bowel symptoms
Despite analgesics, medications, and injections, the pain did not improve.
Persistent, severe back pain in elderly patients must always be thoroughly evaluated to rule out infection, malignancy, or structural instability.
What Did the MRI Reveal?
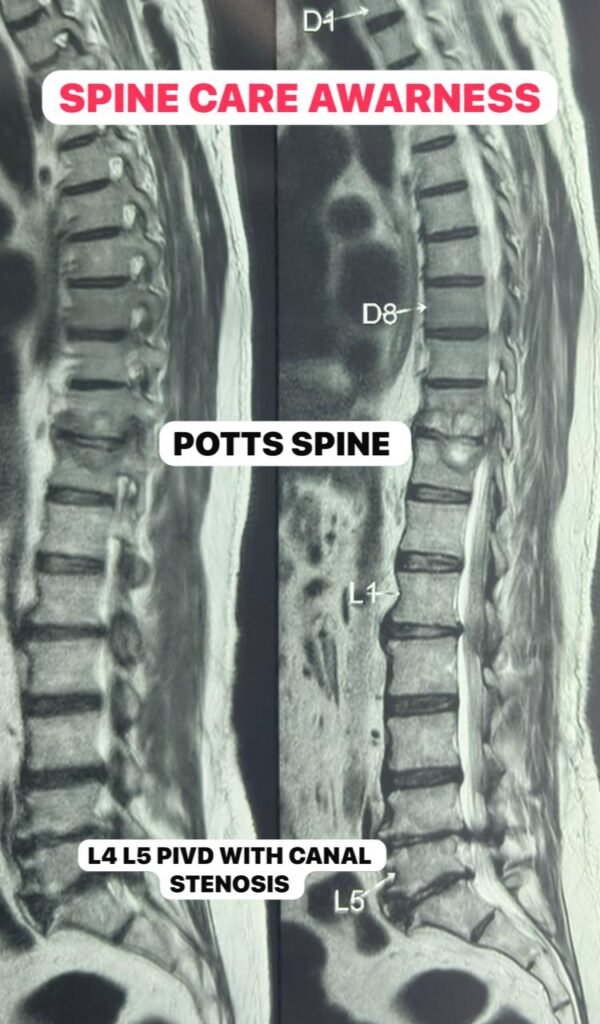
MRI of the thoracic spine showed:
• Soft tissue mass at D8–D9 level
• Significant spinal cord compression
• Destruction of D8 and D9 vertebral bodies
• Structural instability
These findings were highly suggestive of spinal tuberculosis (Pott’s disease).
Additionally, imaging revealed severe lumbar canal stenosis at L4–L5, further increasing the risk of neurological compromise.
What Is Spinal Tuberculosis (Pott’s Spine)?
Spinal tuberculosis is a bacterial infection caused by Mycobacterium tuberculosis that affects vertebral bones and intervertebral discs.
It can:
• Destroy vertebral bodies
• Form abscess or pus collections
• Compress the spinal cord
• Cause paralysis
• Lead to bladder and bowel dysfunction
In India, due to the high burden of tuberculosis, spinal TB remains a major cause of non-traumatic spinal cord compression.
Early diagnosis is critical to prevent permanent disability.
What Happens When Treatment Is Delayed?
Due to delay in appropriate spinal tuberculosis treatment in Bengaluru, the patient developed:
• Progressive numbness in both legs
• Increasing weakness
• Inability to walk
• Complete paraplegia
• Urinary retention requiring catheterization
• Increased pus collection
• Extension of infection
• Severe dorsal spinal cord compression
• Worsening lumbar canal stenosis
The condition had now progressed to a neurological emergency requiring emergency spine surgery in Bengaluru.
When Is Emergency Spine Surgery Required?
Emergency spine surgery in Bengaluru becomes necessary when:
• There is progressive spinal cord compression
• Neurological weakness develops
• Abscess formation threatens neural structures
• Structural instability risks vertebral collapse
• Conservative treatment fails
Delays at this stage may result in permanent paralysis.
What Surgical Procedures Were Performed?
Thoracic Decompression and Fixation
(Thoracic Spinal Cord Compression Treatment)
• Removal of pus
• Decompression of the spinal cord
• Stabilization with pedicle screw fixation
• Reconstruction due to vertebral body destruction
This formed the critical component of Pott’s spine surgery in India for this patient.
Lumbar Canal Stenosis L4-L5 Surgery
• Decompression of nerve roots
• Relief of severe canal stenosis
• Lumbar fusion surgery for spinal stability
The infected material was sent for culture and sensitivity testing.
Based on laboratory results, appropriate anti-tubercular therapy (ATT) was initiated.
How Did the Patient Recover?
Postoperative recovery showed:
• Motor power improved from Grade 2 to Grade 3
• At discharge, Grade 4 power was achieved
• Gradual recovery of bladder function
• Further improvement expected with physiotherapy and rehabilitation
This case demonstrates that even severe paralysis due to spinal tuberculosis can improve significantly with timely surgical intervention.
What Are the Warning Signs of Spinal Tuberculosis?
Consult a spine infection specialist in Bengaluru if you experience:
• Persistent back pain lasting more than 4 weeks
• Night pain
• Pain worsening on coughing or sneezing
• Unexplained weight loss
• Progressive weakness in legs
• Numbness
• Difficulty passing urine
Early consultation with a qualified neurosurgeon can prevent irreversible neurological damage.
How Does Lumbar Canal Stenosis (L4–L5) Add Risk?
Lumbar canal stenosis at L4–L5 may cause:
• Leg pain while walking
• Reduced walking distance
• Numbness and weakness
• Progressive neurological deficits
In severe cases, lumbar canal stenosis L4-L5 surgery provides long-term relief and functional recovery.
Why Early Spine Infection Treatment Matters
Without early spinal tuberculosis treatment in Bengaluru, complications may include:
• Permanent paralysis
• Severe spinal deformity
• Vertebral collapse
• Lifelong disability
Early diagnosis, surgical decompression when required, and complete anti-tubercular therapy are essential to prevent catastrophic neurological outcomes.
Who Should Consult a Spine Infection Specialist in Bengaluru?
You should seek expert evaluation if:
• Back pain persists despite treatment
• MRI shows vertebral destruction
• Weakness or numbness develops
• Walking becomes difficult
• Bladder symptoms appear
• You have a history of tuberculosis
Prompt evaluation ensures accurate diagnosis and timely intervention.
Get Expert Spine Infection Treatment in Bengaluru
If you or a loved one is experiencing persistent back pain, neurological weakness, or signs of spinal infection, early intervention is critical.





Delaying care can lead to permanent neurological damage.
Consult Dr. Ganesh Veerabhadraiah
Dr. Ganesh Veerabhadraiah
HOD & Consultant Neurosurgeon
Kauvery Hospital, Electronic City, Bengaluru
With extensive experience in managing complex spine infections, spinal instability, and emergency decompression procedures, Dr. Ganesh provides specialized care tailored to each patient’s condition.
Visit: Neurowellness
Early intervention can restore mobility and prevent permanent disability.
FAQs
1. What is spinal tuberculosis (Pott’s spine)?
Spinal tuberculosis is a form of tuberculosis infection affecting vertebral bones and discs. It can cause bone destruction, abscess formation, spinal cord compression, and paralysis if untreated.
2. What are the early symptoms of spinal tuberculosis?
Early symptoms include persistent back pain, night pain, pain on coughing or sneezing, mild fever, and weight loss.
3. Can spinal tuberculosis cause paralysis?
Yes. Untreated spinal TB can compress the spinal cord, causing weakness, numbness, bladder dysfunction, and paralysis.
4. When is surgery required for spinal tuberculosis?
Surgery is required when there is spinal cord compression, neurological weakness, instability, abscess formation, or failure of conservative treatment.
5. What does spinal tuberculosis surgery involve?
Surgery may include decompression, removal of infected tissue, stabilization with pedicle screws, and spinal fusion.
6. Is recovery possible after paralysis due to spinal tuberculosis?
Yes. Timely surgery combined with anti-tubercular therapy and physiotherapy can result in significant recovery.
7. What is lumbar canal stenosis (L4–L5)?
Lumbar canal stenosis is narrowing of the spinal canal at L4–L5, causing leg pain, weakness, and walking difficulty.
8. How is spinal tuberculosis diagnosed?
Diagnosis involves MRI, CT scan, blood tests, and culture testing of infected tissue.
9. How long is anti-tubercular treatment required for spine tuberculosis?
Anti-tubercular therapy is usually required for 9–12 months under medical supervision.
10. When should I consult a neurosurgeon for back pain?
Consult a neurosurgeon if you have persistent back pain, weakness, numbness, walking difficulty, bladder issues, or pain not improving with medication.
Conclusion
Severe back pain should never be ignored, especially when it persists despite treatment.
Spinal tuberculosis and degenerative spine diseases are treatable conditions, but delay can lead to catastrophic neurological outcomes.
Timely evaluation, emergency decompression when required, and expert surgical care can restore mobility, preserve bladder function, and significantly improve quality of life.
Early spinal tuberculosis treatment in Bengaluru can save function — and sometimes lives.