Understanding Disc Prolapse and Why Symptoms Matter
Have you ever experienced persistent back or neck pain that doesn’t seem to go away? It might not just be a regular strain—it could be disc prolapse, a condition where the soft, gel-like cushion between your spinal bones slips out of place.
Also known as a herniated disc or slipped disc, this issue can cause nerve compression, leading to discomfort, numbness, and even mobility challenges. Whether due to aging, poor posture, or sudden injuries, disc prolapse is a common yet often overlooked spinal condition.
Recognizing early symptoms is crucial because untreated disc prolapse can worsen over time, leading to chronic pain or, in severe cases, the need for surgery. Many people dismiss lower back pain or stiffness as routine discomfort, but persistent symptoms could indicate deeper spinal problems.
Early diagnosis not only helps in managing pain effectively but also prevents long-term damage to the spine and nervous system. If addressed early, non-surgical treatments like physiotherapy, posture correction, and lifestyle modifications can significantly improve recovery.
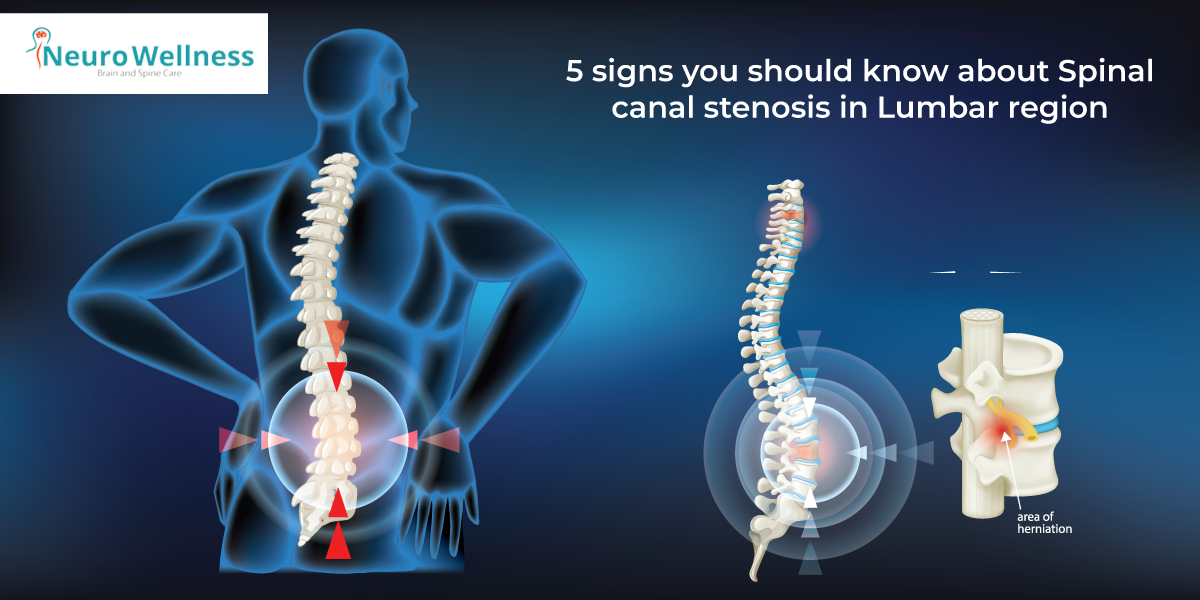
Disc prolapse can affect different areas of the spine, mainly the lower back (lumbar region) or the neck (cervical region), with symptoms varying based on the affected nerves. Lumbar disc prolapse often leads to radiating leg pain (sciatica), while cervical disc prolapse can cause shoulder pain, headaches, or numbness in the arms.
Understanding the warning signs is the first step to protecting your spinal health. If you’re unsure whether your symptoms are linked to a slipped disc, learn more in our detailed guide on What is a Slip Disc?.
Early Signs of Disc Prolapse: Symptoms You Shouldn’t Ignore
Recognizing the early signs of disc prolapse is essential to prevent long-term spinal complications. Symptoms can start mildly and gradually worsen if left untreated. Identifying these warning signs early allows for effective management through physiotherapy, posture correction, and lifestyle changes.
Mild Symptoms (Early Warning Signs)
• Occasional lower back pain or stiffness – You may feel discomfort after long hours of sitting or standing.
• Radiating pain in arms or legs – Pain may travel down the limbs due to nerve compression.
• Numbness or tingling sensations – Affected nerves can cause a “pins and needles” feeling in hands, fingers, feet, or toes.
Learn more about early symptoms in our article on Signs of Lumbar Disc Prolapse.
Moderate Symptoms (Progressing Disc Prolapse)
• Pain worsening after prolonged sitting – Sitting for long periods can increase pressure on the spinal discs, intensifying pain.
• Weakness in legs, arms, or hands – Muscle weakness may indicate nerve irritation, reducing mobility and grip strength.
• Reduced flexibility in the spine – Difficulty bending, twisting, or stretching may suggest increased disc degeneration.
Ignoring these symptoms can lead to severe nerve damage and chronic pain, making early intervention essential. If these symptoms persist, consulting a spine specialist is recommended.
Expert Explains: Key Symptoms of Disc Prolapse
Disc prolapse can affect your quality of life—but recognizing early signs can help you avoid long-term complications. In this short video, Dr. Ganesh Veerabhadraiah, one of Bangalore’s top neurosurgeons, breaks down the core symptoms of disc prolapse that should never be ignored.
With 20+ years of experience in spine and neurological surgery, Dr. Ganesh is renowned for his expertise in minimally invasive spine procedures and patient-first care. His insights are backed by decades of clinical experience and successful outcomes.
Watch the video to hear directly from the expert:
4 Reasons Why Disc Prolapse happens?
1. Age-Related Degeneration
2. Poor Posture & Sedentary Lifestyle
3. Heavy Lifting with Wrong Technique
4. Sudden Injury or Trauma
Accidents, falls, or jerky movements
Symptoms of Disc Prolapse in the Lower Back & Neck
The location of the disc prolapse determines the type and severity of symptoms. While lumbar disc prolapse primarily affects the lower back and legs, cervical disc prolapse impacts the neck, shoulders, and arms. Identifying these symptoms early can help in seeking the right treatment before the condition worsens.
Learn more about cervical disc issues in our detailed article on Know About Disc Prolapse at Neck (Cervical PIVD).
Lower Back (Lumbar Disc Prolapse) Symptoms
• Severe lower back pain that spreads to the legs (sciatica) – The slipped disc may press on the sciatic nerve, causing pain that radiates down one or both legs.
• Difficulty in standing, bending, or lifting objects – Everyday movements become painful due to spinal instability and nerve irritation.
• Loss of reflexes in the legs – Nerve compression can reduce sensation, making your legs feel weak or unresponsive.
Neck (Cervical Disc Prolapse) Symptoms
• Pain in the shoulders, arms, and hands – Nerve compression in the cervical spine can cause discomfort and weakness in the upper body.
• Neck stiffness and limited movement – Reduced flexibility can make it difficult to turn your head, causing discomfort while driving or working.
• Headaches and dizziness due to nerve compression – Irritated cervical nerves may trigger persistent headaches and balance issues.
Ignoring these symptoms can lead to chronic nerve damage and reduced mobility. If you’re experiencing persistent pain, it’s best to consult a spine specialist near you for early intervention.
Warning Signs That Require Immediate Medical Attention
While mild to moderate disc prolapse symptoms can often be managed with conservative treatments, some warning signs indicate a serious medical emergency. If you experience any of the following symptoms, seek urgent medical attention to prevent permanent nerve damage or disability.
Read about surgical options and how they help in recovery: How Spine Surgery in India is Helping Patients with Chronic Back Pain.
Seek Urgent Medical Help If You Experience:
• Loss of bladder or bowel control (Cauda Equina Syndrome – Medical Emergency) – This rare but serious condition occurs when nerves at the base of the spine are severely compressed, leading to incontinence and loss of sensation in the lower body. Immediate surgery is often required.
• Sudden paralysis or complete numbness in legs or arms – A complete loss of sensation or muscle function in the limbs indicates severe nerve damage, which can become permanent if not treated promptly.
• Sharp, persistent pain that doesn’t improve with rest or medication – If your pain is severe, continuous, and resistant to pain relief methods, it may signal a worsening condition requiring medical intervention.
Ignoring these warning signs can lead to permanent nerve damage, disability, or loss of function. If you notice these symptoms, contact a spine specialist immediately to explore urgent treatment options.
How to Know If You Have a Prolapsed Disc?
Identifying a prolapsed disc early is crucial to prevent worsening symptoms and long-term nerve damage. While only a medical professional can confirm a diagnosis through MRI or CT scans, you can perform some self-assessment tests at home to check for possible signs. These tests help evaluate nerve function, muscle strength, and pain response.
Learn more about protecting your spine from further damage: Guarding Your Back: Expert Methods to Halt the Progression of Back Pain.
Self-Assessment Tests
🔹 Pain Trigger Test – Pay attention to when your pain worsens.
✔ If pain increases while sitting, bending forward, or lifting objects, it may indicate lumbar disc prolapse.
✔ If neck pain worsens with head movements or long screen time, it may suggest cervical disc prolapse.
🔹 Reflex & Strength Test – Check for muscle weakness.
✔ If you experience weakness in your legs, arms, or grip strength, your nerves may be compressed.
✔ Difficulty standing on your toes or heels could be a sign of nerve dysfunction due to a herniated disc.
🔹 Sensation Test – Detect nerve compression effects.
✔ If you feel numbness, tingling, or a pins-and-needles sensation in your arms, hands, legs, or feet, your spinal nerves might be affected.
✔ A burning or radiating pain down one leg (sciatica) is a common symptom of lumbar disc prolapse.
If you experience any of these symptoms persistently, consulting a spine specialist near you is the best step for an accurate diagnosis and treatment plan. Early intervention can help you avoid surgery and manage the condition effectively.
When to See a Spine Specialist for Disc Prolapse?
If your back or neck pain persists for more than six weeks despite home treatments like rest, stretching, or physiotherapy, it may be time to see a spine specialist. Symptoms that worsen with movement, radiate down the arms or legs, or interfere with daily activities could indicate progressive nerve compression that requires professional care.
Experiencing balance issues, difficulty walking, or muscle weakness in your limbs could be signs of a severe disc prolapse needing urgent evaluation. Consulting a top spine specialist in Electronic City, Bangalore, ensures access to advanced diagnostic tools and personalized treatment options. Find expert care at Brain and Spine Clinic, Electronic City, Bangalore.
Treatment & Management Options for Disc Prolapse
Early treatment can help manage disc prolapse effectively and prevent the need for surgery. Non-surgical methods like physiotherapy, posture correction, and pain management techniques are often the first line of treatment, helping patients regain mobility and reduce discomfort naturally. By making lifestyle changes and following expert recommendations, many people can recover without invasive procedures.
However, in severe cases where nerve compression leads to persistent pain, weakness, or loss of function, minimally invasive spine surgery may be necessary. Procedures like microdiscectomy help relieve pressure on spinal nerves, while spinal fusion stabilizes the spine in advanced cases.
Learn more about spine health and prevention tips in our guide: 20 Tips to Prevent Disc Prolapse.
Non-Surgical Treatments
✔ Physiotherapy & targeted exercises – Strengthens core muscles to support the spine and relieve pressure on discs.
✔ Posture correction & ergonomic support – Helps prevent worsening of symptoms through proper body mechanics.
✔ Pain relief techniques – Heat therapy, acupuncture, and medications can ease discomfort and inflammation.
Surgical Treatments (If Required)
✔ Microdiscectomy – A minimally invasive procedure to remove the herniated portion of the disc, relieving nerve pressure.
✔ Spinal fusion – Recommended for severe cases to stabilize the spine and prevent further damage.
Seeking early intervention and following a personalized treatment plan can help manage disc prolapse effectively, ensuring better spine health and long-term recovery.
How to Prevent Disc Prolapse and Maintain Spine Health
Preventing disc prolapse starts with maintaining good posture, regular movement, and proper spinal care. Using an ergonomic chair, practicing correct sitting posture, and avoiding long hours of slouching can reduce strain on the spine. Staying physically active with low-impact exercises like swimming, yoga, and core strengthening helps support spinal stability. Additionally, always lift heavy objects with proper technique to avoid unnecessary pressure on the lower back.
For more spine care tips, check out
Final Thoughts: Prioritize Your Spine Health
Taking care of your spine health is essential to prevent long-term complications like chronic pain and mobility issues. Early diagnosis and timely intervention can help manage disc prolapse effectively, reducing the need for invasive treatments. If symptoms persist or worsen, consulting a spine specialist ensures the best course of action for recovery.
Prevention is always better than cure—adopting a healthy lifestyle, maintaining good posture, and staying active can go a long way in protecting your spine. Listening to your body and seeking medical advice when needed can help you lead a pain-free, active life. If you’re experiencing symptoms, book a consultation with a spine specialist in Electronic City at the best Brain and Spine Clinic
Author– Dr Ganesh Veerabhadraiah, Consultant Neurosurgeon- Brain & Spine
FAQ
1. What are the early symptoms of disc prolapse?
Mild back pain, stiffness, and discomfort while bending are early warning signs.
2. How is disc prolapse diagnosed?
Through MRI, CT scan, and neurological examination by a spine specialist.
3. Can disc prolapse heal without surgery?
Yes, mild to moderate cases improve with physiotherapy, medications, and posture correction.
4. When is surgery needed for disc prolapse?
If symptoms worsen or there is nerve compression, surgery like MISS or ACDF may be required.
5. Where can I get disc prolapse treatment in Bangalore?
Neurowellness Brain & Spine Clinic provides advanced disc prolapse care with expert neurosurgeons.

About Author
Dr. Ganesh Veerabhadraiah
Dr. Ganesh Veerabhadraiah, leading neurosurgeon and neurologist in Bangalore, has over 20 years of expertise in managing back pain, migraines, headaches, neuro disorders, and spine problems. His clinical excellence and patient-first approach make him one of the most trusted neuro doctors in Bangalore.
At Neurowellness Brain & Spine Clinic in Jayanagar and Kavery Hospital Electronic City, Dr. Ganesh provides comprehensive treatments ranging from minimally invasive spine surgery to advanced neurological care. As a respected back pain specialist and migraine doctor, he continues to deliver reliable outcomes for patients.
👉 Connect with Dr. Ganesh on LinkedIn